By Jessica Firger
It's estimated that some 2.2 million Americans have glaucoma, a condition that damages the optic nerve and is the leading cause of blindness worldwide, but only half know they do. In the United States, more than 120,000 people are blind from the condition, according to the Glaucoma Research Foundation.
But the U.S. Preventive Services Task Force, the panel of health care experts that reviews screening guidelines for common health conditions such as breast or prostate cancer, remains skeptical about screening for glaucoma. In a statement released this week, the agency said more research must be conducted to assess whether screening for open-angle glaucoma by primary care physicians would actually improve patient outcomes or reduce incidence of the disease.
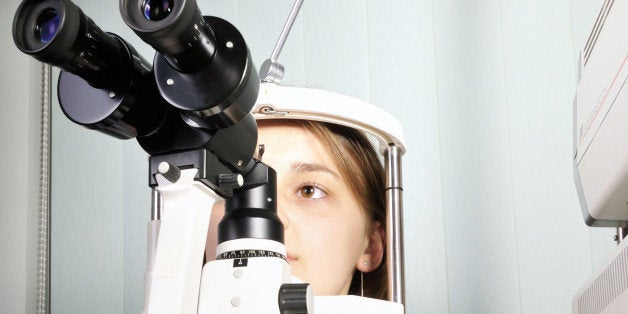
How Doctors Screen for Glaucoma
Many eye specialists argue that rates of glaucoma could be reduced if more patients were screened. Some suggest that if screenings were routinely conducted by general practitioners, the disease -- which has few symptoms until late in its course -- would most likely be caught earlier and successfully treated.
More from Everyday Health:
Depressed Persons More Likely to Set Abstract Goals
Oh, Yummy Mummies: High Standards for Celeb Moms Like Kim Kardashian
Jeff's Story: A Patient's Experience With Heart Failure
The most basic screening for glaucoma is a test of eyeball pressure, and it can be done by an optometrist during a routine exam, or by an ophthalmologist. The eye specialists uses a technique called tonometry to measure the pressure in both eyes. This is typically done through an air puff or noncontact tonometer, or applying numbing drops to the eye and using using a tonometer that touches the eye's surface to measure resistance. A primary care physician most likely would use a much simpler hand instrument.
For further screening, an eye specialist puts special drops in the eyes that temporarily enlarge the pupils, affording a better inside view of the eye and the optic nerve to check for damage. The specialist may also use visual field testing to assess side and peripheral vision loss. Certain imaging techniques, such as tomography and magnetic resonance imaging, may also be used to screen for the disease.
Why Not Screen Everyone for Glaucoma?
"We found that the evidence wasn't convincing that there were accurate ways for screening for glaucoma in primary care," said Albert Siu, MD, Task Force co-vice chairman and professor and chairman of geriatrics and palliative medicine at Mount Sinai Hospital in New York City. "We could not make a recommendation one way or another, in terms of whether primary care physicians should screen for glaucoma." Dr. Siu said there isn't data on the frequency of glaucoma screenings in primary care settings, though he suspects the practice is uncommon.
Pam Sheffield, MD, a family doctor and clinic chief at the University of Washington neighborhood clinic in Belltown and Ravenna, said years ago her practice looked into offering glaucoma screenings onsite, but decided against it for fear that it might be challenging to properly maintain and clean the equipment. Instead her doctors encourage interventions from specialists.
"We're trying to get more optomotrists in our clinics because they can do those more advanced screenings," said Dr. Sheffield. She added that unless a patient is diabetic, her clinic doesn't track eye screenings.
"It is something I routinely recommend in my practice but you're not going to get a letter from me saying 'hey, you didn't get your eye screening done.'"
The American Academy of Ophthalmology recommends individuals receive a baseline eye examination beginning at age 40, and be screened annually starting at age 65, as well as a number of other eye conditions. However, most doctors agree that certain patients should be screened regularly for the disease.
"If a patient is at higher risk for glaucoma, such as African Americans or Latinos, then some consideration should be made as to whether they should see an eye specialist periodically," said Siu. After cataracts, glaucoma is the leading cause of blindness among African Americans.
A Symptomless Condition With a Serious Outcome
The Task Force's review specifically applies to open-angle glaucoma, the most common type of the disease, and is focused on patients who don't currently have vision problems. But open-angle glaucoma, also called the "silent thief of sight," does not exhibit any symptoms until later in its course, which makes it especially difficult to detect and treat.
Patients with symptoms of the disease typically present with pain from elevated eye pressure and loss of vision, especially decreased peripheral and side vision. In its more advanced stage, glaucoma causes tunnel vision, which is a complete loss of peripheral and side vision, though the person usually maintains central vision.
Currently, there is no cure for glaucoma. But if elevated high pressure is detected early, there are effective treatments. There are a variety of eye drops that work to decrease pressure in the eyes and lower the risk of damage to the optic nerve. Laser surgery can also lower intraocular pressure, which is the pressure exerted by the fluids inside the eyeball.
"If there are symptoms, the disease progresses really slowly, and it may start with what doctors call visual defects, or a blind spot, and it's usually really isn't noticed by a patient," said Siu.
The Task Force recommends further research on glaucoma screening and prevention. Until then, the group suggests patients and doctors use their own judgement to monitor possible development of the disease. "Certainly if there are visual complaints a referral should be made to an eye specialist." said Siu.
"Glaucoma Screening: Is a Task Force Blind to the Facts?" originally appeared on Everyday Health.
