Last June saw the arrival of the Nutrition for Growth Summit in London, an exciting and ambitious event leading up to the 2013 G8 Summit. One of the major outcomes of this gathering was the endorsement by 90 stakeholders representing government, business, science and NGO leaders from around the world of a compact to significantly reduce global hunger by 2020 and a stunning $4.15 billion financial commitment to help realize that goal.
Last week, Canadian Prime Minister Stephen Harper convened another global summit in Toronto on maternal, infant and child health. The role of nutrition was deemed so important to success in this area that a plenary panel was organized to discuss how to step up financial commitments and expand nutrition work on the ground. I had the honor of being the sole U.S. representative on this panel. At the end of summit, Prime Minister Harper announced that Canada is committing another $3.5 billion over five years to improve global programs in maternal, infant and child health. That's on top of the $2.85 billion they committed in 2010 while hosting the G8 summit -- tremendous commitment in support of this work!
While it is always a privilege to participate in such high-level forums and learn from other leaders in global development, in preparing for this latest event I could not help but steer the dialogue toward one of the most crucial elements in making the big picture plans a reality: the local health professionals working in some of the poorest communities in the world. Their role in reaching populations in need is essential, yet developing their capacity to do so remains one of the greatest challenges to achieving the larger goals we set in the fight against hunger and malnutrition.
To ensure the sustainability of the impact of nutrition programs, we must do more to develop the capacity and knowledge of local nutrition workforces in high burden countries. We need to build national capacity in designing and implementing state-of-the-art programs before we can expect to make any significant, lasting gains in improving nutrition among mothers and children.
While there has been some investment in training doctors, nurses, clinical officers, nutritionists and others as part of in-service programs, there remains a huge need for pre-service training on what nutrition actions and interventions work with target communities.
Right now, even within the existing in-service training, knowledge has been delivered in silos so that health workers are not prepared to provide the entirety of support needed at various key points in the lifecycle. For example, a health worker might receive training in emergency feeding but never learn about micronutrient supplementation or appropriate complementary feeding, two practices recognized as key to decreasing child mortality rates in impoverished communities.
A typical scenario today might involve a pregnant woman who attends an antenatal clinic, but never receives advice regarding her diet during pregnancy or the importance of taking iron folate tablets or deworming pills. She will likely not even receive counseling to prepare her to initiate breastfeeding in the first hour of her baby's life. While this additional counseling may be available through other services, we cannot expect this woman, who may have traveled miles on foot just to take advantage of that single health visit, to return for separate visits for each area.
This is why Helen Keller International has promoted an integrated approach to training of community health workers, something known as the Essential Nutrition Actions, which promote healthy nutrition throughout the lifecycle -- ensuring that the right nutrition support is given to the right person at the right time in the right way.
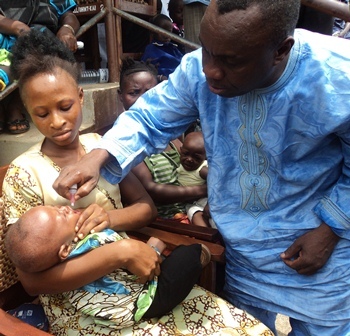
We see this more comprehensive approach working in our programs. In Sierra Leone, through the support of the Canadian and Irish governments as well as UNICEF, we've succeeded in integrating a health center visit for six-month old infants so they can receive their first vitamin A supplement on time. Simultaneously, their mothers can receive counseling on infant and young child feeding and family planning, and the children and their caregivers can catch up on any missed vaccinations. The response on the community level has been overwhelmingly positive and we are exploring ways to bring this model to other countries.
Equally important to the transfer of this knowledge, health professionals need to be trained so that they develop effective interpersonal communication and negotiation skills to ensure that their knowledge can be translated into action.
These health workers are the people mothers look to for advice. They are the people who will be sitting with a new mother to ensure her newborn is put on the breast during the first hour of life and explain why she should exclusively give her child breast milk during the first six months. These are the people that, after those six months, will teach a new mother what kinds of complementary foods are best to feed her child.
Some of this new knowledge will be different than what families are used to. Thus, the road to good nutrition involves educating and negotiating with mothers, as well as their fathers, in-laws and other community members to adopt and support ongoing healthier practices.
If we fail to start making more meaningful investment in this kind of capacity development now, we may well find ourselves still struggling with inadequate health systems and limited human resource capacity not only come 2020, but 20 years down the road and beyond.
The good news is that we are primed to move positively in the right direction. The Nutrition for Growth Summit and other recent initiatives throughout the global community have raised unprecedented levels of funding for nutrition programming and there is now a coordinated global effort through the Scaling Up Nutrition (SUN) Movement. We are seeing increased consensus among global partners, researchers and country implementers on the goal of reducing hunger and on what interventions are needed to deliver proven interventions at scale.
The next step toward success should be ensuring that this promising climate be bolstered by the best possible models for sustainable and country-owned and locally-led delivery. When local health professionals receive pre-service training that stresses how to better leverage opportunities to educate and instill good behaviors in mothers and children at every health visit, instead of project-specific events, we can better promote and sustain positive nutrition practices during the first 1,000 days of life, as well as other key points in the development cycle.
Reducing malnutrition around the world is a conceivable and urgent objective that we must commit to in order to break cycles of poverty and build a better future for women and children.
This post is part of a blog series in partnership with 1,000 Days to highlight global momentum for nutrition. Click here to view the entire series.