👀 DON'T MISS 👀
The children's responsibilities included cleaning kill equipment — head splitters, jaw pullers, bandsaws and neck clippers — the Labor Department said.
“The negligence and the arrogance and the lack of accountability is manifesting itself into the last neighborhood of the Gaza Strip," an evacuated American says.
The administration will soon send a report to Congress on whether Israel is violating U.S. and international law by using American weapons to kill civilians.
Vladimir Putin is beginning his fifth term as Russian president after destroying his political opposition, launching a devastating war in Ukraine and consolidating power.
Wesley Bell raised more than $65,000 from donors who also gave to several Missouri Republicans.
Israel has brushed off urgent warnings from allies and humanitarians against launching an invasion into the city home to over a million Palestinians.
In a series of TikTok videos, 26-year-old Eugenio Casnighi says he was dismissed after a clip in which he appeared alongside Kylie Jenner drew thirsty comments.
The Democrat said she “misspoke and I regret it” after her comments were condemned as “harmful, deeply uninformed and genuinely appalling.”
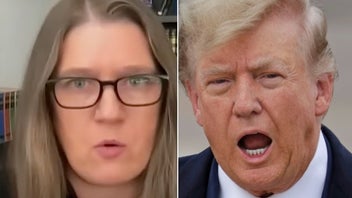
Many reactions to the news of Trump's trip went along the lines of "told you so."
The name change to Scouting America comes as the organization emerges from bankruptcy following a flood of sexual abuse claims and seeks to focus on inclusion.
The "Roar" singer has attended the annual fashion event for years, but was notably absent this time.
The Alabama native has been grinding in Nashville for eight years — now, she’s on the cusp of releasing her first full-length album.