"Beyond The Battlefield" is a 10-part series exploring the challenges that severely wounded veterans of Iraq and Afghanistan face after they return home, as well as what those struggles mean for those close to them. Learn how you can help here. Other stories in the series can be found here. Listen to reporter David Wood discuss "Beyond The Battlefield" with NPR's Terry Gross here.
It was just another hot, dusty August day in Kabul five years ago, and Army Staff Sgt. Todd M. Nelson was traveling in just another convoy passing just another of the thousands of white Toyota Corollas that crowd Afghanistan’s capital. Except this Corolla was packed with explosives, and as Nelson's convoy passed, the suicide driver detonated them.
The blast blew the Corolla to bits and shredded the right side of the Toyota Land Cruiser where Nelson was sitting. The shock wave crushed his face, smashing the bones behind his cheeks, his forehead and his chin and nose. Jagged chunks of metal and glass slashed across his face, ripping off flesh and muscle and tearing away bone fragments. A fireball followed, searing his right arm, setting his head aflame beneath his helmet, burning off his nose and ears and eyelids, then charring what was left of his face.
A decade ago, Nelson would have had a slim chance of living after a blast like that. Recent major improvements in battlefield trauma care, swift medical evacuation and advances in burn surgery and reconstruction saved his life.
But it was close: When he arrived at the burn center at Brooke Army Medical Center (BAMC) in San Antonio, he was in a coma and the only evidence that he was still alive was his beating heart.
"These are particularly disturbing injuries," says Dr. Robert G. Hale, who performed many of the dozens of surgeries on Nelson's face in San Antonio. After the charred flesh is washed away with gentle streams of warm water, the wound has to be covered with skin grafts to prevent life-threatening infection, which can set in quickly. "If you don't close the wound within a month or two, many of these patients don't make it," Hale says.
Once the burn is covered, there's no way to operate to try to reconstruct the face without taking the skin back off -- or by burrowing through nearby flesh.
Meanwhile, as the skin graft heals, it contracts into painfully thick scars, pulling soft tissue such as eye openings, nostrils and mouths into grotesquely distorted shapes as it shrinks unevenly across the face. Each subsequent surgery forms more scars, with more painful shrinking and more contortions. Nelson's contracting scars flattened his nose, turned his one eyelid inside out and pulled down the corners of his mouth.
Trying to correct these distortions and enable severely burned patients to make normal facial expressions requires months and years of painful and debilitating surgeries, with outcomes often less than ideal. At some point most patients simply decide, as Nelson did, that enough is enough and wave off more surgery.
But that was years away. First, doctors cleaned and covered his wounds, and performed dozens of innovative surgeries to restore Nelson’s face to a form acceptable to him. In one series of operations, Hale pieced together the bone fragments of his jaw by operating through incisions inside Nelson’s mouth and neck.
From the very edge of death, Nelson was given new life -- and he seized the opportunity.
WARNING: Graphic images of medical procedures appear in the slideshow below.
Less than four months after he arrived in San Antonio in a coma, Todd Nelson walked onto the dance floor at the BAMC holiday ball with his wife, Sarah. His face at that point was still grotesquely disfigured. But he wore an American flag bandana tied proudly over his burned skull and his best dress uniform as he and Sarah swirled and turned among the dancers.
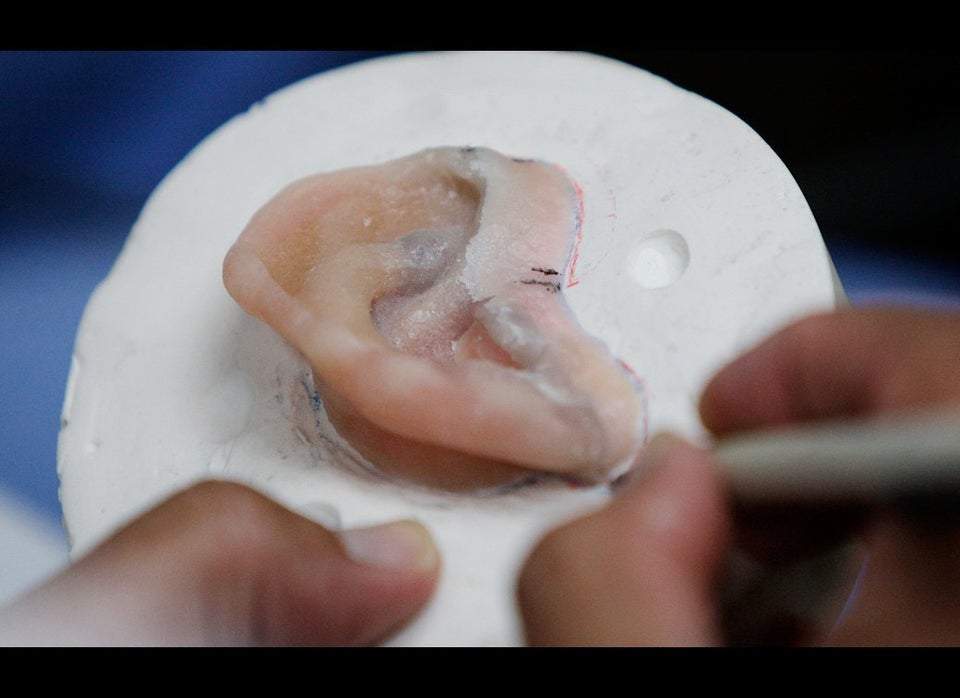
Over four years, Hale and other surgeons performed 43 surgeries on Nelson, leaving his face a patchwork of scar tissue and grafts of his own skin as well as synthetic skin, pig skin and cadaver skin. He has a prosthetic eye and a prosthetic ear that attaches with magnets to a metal plate in his head. ("I've almost lost it a couple of times," he says with a sheepish grin. "I got a backup ear, but it's one of those things you gotta worry about.")
Nelson can see and hear and speak normally, and he's gotten used to going out in public. That's a long way from his first glimpse of himself in the mirror after he was wounded. "I looked like Skeletor," he recalls. "All I could think to myself was, ‘I guess I can live with this.’ Because I felt fortunate just to be alive."
Yet Nelson's case also marks a limit as to what modern medicine can presently achieve. "There is no way to return these patients to function and aesthetics," Hale says. "We have run out of options with conventional treatment."
Even face transplants have proven less than satisfactory. Since 2005, when French surgeons performed the world's first facial transplant, the Defense Department has funded all five full facial transplant operations for American patients. The procedure sentences the patient to a lifetime of immuno-suppression treatment. "Once they stop that medicine, whatever body part you gave them from somebody else will be rejected," Hale points out.
Frustration with this apparent dead-end has led Hale and many others into a fast-paced research effort to perfect new techniques in regrowing the patient's own tissue. Hale is director of craniomaxillofacial (head, jaw, face) research at the U.S. Army Institute of Surgical Research in San Antonio and a consultant at the Armed Forces Institute of Regenerative Medicine.
He and other military researchers are working with scientists at the Department of Veterans Affairs, the National Institutes of Health and the Uniformed Services University of the Health Sciences in Bethesda, Md., and universities across the country to regenerate tissue lost in combat -- skin, muscle, bone, blood vessels, even nerves.
Some of their work, including human-engineered skin and spray-on skin made from a patient's own stem cells, will be put through clinical trials shortly aimed at winning a stamp of approval from the Food and Drug Administration. That may only be the beginning.
"Twenty years from now, I think we will be able to regenerate the entire face," Hale says.
THEIR SKIN WAS GONE
Hale, 54, was a highly successful surgeon with a booming practice in Los Angeles when he was summoned in 2003, as an Army reservist, to active duty as a trauma surgeon. Working in a field hospital in Kuwait, he experienced the first waves of the severely wounded as the Iraq war ignited into a raging and bloody insurgency. There were few surgeons on hand, and even fewer with his special skills in facial and jaw reconstruction.
"I saw soldiers with horrific injuries that conventional treatment could not even hardly close, much less make functional," he says.
Recognizing both a need and a calling, he instructed his wife to sell his lucrative private practice back home. Hale stayed on active duty, serving another tour in Afghanistan where there was such a shortage of medical staff that he treated his own infected tooth by pulling it himself, using forceps and a mirror.
Returning home to work with burned soldiers and Marines, Hale kept running across an ugly problem: Many of them were burned so badly that their skin was gone -- and with it the underlying layers of fat, muscle and other tissue that is essential in bringing blood to a skin graft sewn on top. Without blood and nourishment from underlying fat, grafted skin will die.
To get around the problem, Hale eventually performed several surgeries on Nelson and other patients in which he partially cut a piece of skin from one shoulder, sewing an end of it onto a wound and leaving the other end still attached to the shoulder so it could continue to carry blood and other nutrients into the skin.
The surgery would leave Nelson wearing a sheet of skin, or what surgeons call a "flap," with one end still attached to his chest and the other grafted onto his cheek. It would take 20 days for the flap to heal, drawing blood and nutrients from its new site on his face, before surgeons could safely sever the end from Nelson's shoulder.
These surgeries began months into Nelson's treatment. In the meantime he had become an outpatient at BAMC, had bought a nearby house and moved in with his family. While the flaps were healing, with the sheets of skin stretching between his shoulder and cheekbones, regular life went on, for weeks.
"You have to walk around San Antonio -- home improvement, grocery store -- everybody knows you, you look like Jabba the Hutt," Nelson says, a glint of humor in his eye. Asked how difficult that was for him, he shrugs. "You don't do as much socializing in the checkout line."
Nelson’s flap procedures didn't work perfectly. The blood supply tended to run out at the edges of the flap and the skin there would die. The operation produced more scarring and contractions that pulled his mouth out of shape.
"When it comes to skin grafts, it's roll of the dice as to how much of it is going to work and if it's gonna work at all," Nelson says. Above all, the skin didn't look right. The skin on his cheeks, from a graft that eventually did heal, is shoulder skin -- not facial skin.
"There is nothing on the body that looks like a face, except a face,” Hale says.
The reconstruction of Nelson's face went on. Surgeons worked to build an eyelid over his right eye, which he had lost in the explosion, but there's not enough muscle left and it just sags. They tried to build up his nose, using synthetic material to recreate the bridge of his nose, but the skin just shrank and tightened up around it and flattened the nose again. Hale and others tried a surgical technique called a z-plasty, in which the skin graft is cut in the shape of a Z, to minimize the painful and ugly shrinkage around his mouth. But the scars would worsen, and they'd try more z-plasties, and those didn't do any better.
When they could, surgeons would "harvest" a patch of skin from somewhere on Nelson's body, usually from his back. They would try to pull the edges of this new wound together and use expanders to stretch the skin around it. In three weeks, new skin would have formed and be ready to harvest again -- a painful and laborious process repeated over and over.
At the outset of his facial reconstruction, Nelson conferred with the surgeons to plan what would be done. "You have to have a plan because you run out of patience with the process after so many procedures," Nelson recalls. "I told them I wanted my eyelids to close, I wanted to be able to breathe through my nose, to eat a good-sized hamburger. Simple things."
Not, as it turned out, that simple. "It was one step forward and two steps back," Nelson says. Eventually, he "kind of hit the wall," and asked that no more surgeries be done on his face.
"I ended up with some of the best skin I've seen on a burn patient myself," Nelson says. "A lot of folks are nowhere near as fortunate as me. The problem was we were sort of repeating ourselves, almost like a broken record."
Nelson consults regularly with Hale on the research underway, but he is cautious and wary. "I am looking forward to improvements that are really proven," he says, "where if I do a procedure I can see a quantitative result. That's what I'm really looking forward to.
"I would like my nose to be improved. I think that would be probably number one. It's the first thing you see, really. I would love to have an ear back, if I could get another ear …"
THE RESEARCH RACE
While Nelson and others wait, researchers are racing to perfect a wide range of new medical technologies and procedures, among them several initiatives specifically designed for the severely burned:
-- Spray-on skin: In the operating room where they are working on a new burn patient with second-degree burns, surgeons can remove a small, postage-stamp size piece of the patient's skin, extract the skin cells, place them in a solution and spray them on the open wound where they will grow vigorously. The spray-on skin quickly closes a large wound area with the patient's own skin, lowering the risk of infection and eliminating the need for difficult and painful skin grafts. The technique has been shown in Europe to be effective. "It's like throwing seed out on a fertilized field," Hale says. "We know it works." Clinical trials are underway to win FDA approval.
-- Tissue-engineered skin: Third-degree burns leave patients with no layers of skin. To replace "full-thickness'' skin, surgeons remove a patch of a patient's skin and send it to a lab in Rockville, Md., where enzymes are used to break out different types of skin cells that are cultured and grown on a square meter of collagen sponge. Then it's shipped back for surgeons to use. Because it is the patient's own skin, it heals better and is perfectly matched in color and texture, although more work is needed to effectively use it on the face.
-- Adipose fat transfer: The fat that normally underlies the skin often is burned away in a severe wound. Researchers have found that fat taken from elsewhere on the patient's body, enriched with the patient's own adult stem cells and injected under a tissue-engineered skin or a graft helps a wound heal without abnormal scarring.
-- The bio-mask: It is possible, researchers believe, to combine various technologies to create a healing mask for burn patients like Todd Nelson. Step one is a wound-vac, a black foam device connected to a suction pump that is placed on the open wound, where it helps pull the wound edges together and gently draws out excess fluid and infectious material that inhibits healing. Such devices are in use but are not yet adapted for the face.
Next, Hale would apply tissue-engineered skin, inject fat rich with stem cells beneath it, and place over the patient's face a mask made from a three-dimensional CT scan. Very light suction would continue to draw fluid from the wound and encourage the upward growth of blood vessels into the new skin.
When this layer of tissue is healing, rich with new blood vessels, Hale would use spray-on skin to add the final layer of outer skin.
The technical details of the bio-mask have yet to be worked out, but Hale is excited about the promise. "If this process works, you would have a higher-functioning and aesthetic skin," Hale told me. "We have the technologies, we need to tweak them and apply them and prove it works. We think in five to 10 years we will be able to replace a burn patient's face using this bio-mask, fat transfer and the new technologies of skin engineering."
That leaves only one step before surgeons can regenerate a face for Nelson: regrowing muscle. r"Once we know how to regenerate muscle, then we can add it all together 10 to 20 years from now and regenerate the entire face," he says, beaming.
MOVING FORWARD
But Todd Nelson is not the kind of guy to stand around and wait. He's been working on a college degree in education. Some people have asked him to go on a speaking tour; others have suggested government service.
"Whatever it is, I want to be passionate about it," he says. "Life is too short to live for the weekends."
Todd had been married just six months before he deployed to Afghanistan. He was blown up 45 days before the end of his second one-year combat tour. It was his second marriage; his first broke apart during his first combat tour, in Iraq.
His second wife, Sarah, was born with one leg and walks with a prosthesis, which has made for some interesting encounters. At a movie theater recently, the young lad taking the tickets stared at her leg, then at Todd's face. "Wh-wh-what happened?" he gasped.
"We looked at each other and wanted to ask innocently, 'What?' but we didn't, though," Todd said later.
His wife's strength and his faith have pulled him through the ordeal, he told me. And like many of the severely wounded, he has come through it with a brimming optimism and energy. It's as if he has been given a new life.
In war, he said, "you really learn that you are out of control, that this life is not in your control, so you turn to your faith. And that prepared me for this." In Afghanistan he served at the base chapel as a music minister. After he was wounded, he took his guitar to the worship center at BAMC as soon as he could make chords with his fingers, and began leading the music.
"That's really been the cornerstone. I give that all the credit for my positive attitude," he says. "It's the only way you can get through an event regardless of whether it's a suicide bomb or the foreclosure of your house. It's only your attitude, and I think my faith has been what has kept that going."
His severe wounds were hard on Nelson’s two daughters, too. In their young teenage years, they were not immediately allowed to come see him, and his disfigurement was hard to accept. It was particularly hard on his eldest daughter. She became withdrawn, and her grades suffered. "That put the pressure on me. I had to step up and be the dad again," he said. He did, and drew the family together, and her grades went back up.
But not long ago, his former wife, who is remarried, learned that her new baby had leukemia. The news further devastated Nelson's eldest daughter, but they dealt with the crisis and the baby is doing okay.
"But it's, you know, if there's a reason for everything, maybe this [his wound] was to prepare her for her sister's ordeal, and who knows what this is preparing her for in the future? We've just tried to see the silver lining in this kind of thing," Nelson says.
That attitude extends to his Army service. He might have been furious that he was forced to conduct convoys in Afghanistan with "soft-skin" un-armored vehicles, when the threat of IEDs and suicide bombs was evident.
He is not furious.
Todd Nelson has retired from the Army as a master sergeant. It was time. He had enlisted as a "typical misguided teenager" looking for the regular pay and the GI Bill and vocational education as a mechanic. "And I got that," he said. "They gave me everything I ever wanted, and I knew I was taking a chance every time I signed up. When this happened, it was just … the dice finally landed double snake eyes. It was part of the chance I was taking, so I don't harbor any bad feelings toward it. The price had to be paid and it was going to be paid that day … and I was the one to pay the price," he said. "I don't have any beef against the VA or the military medical system. They've been really good to me the whole way."
In addition to faith and family, he draws much of his passion and strength from the response of so many ordinary Americans who have been in touch with him since his injury. He had long aspired to own a Harley Davidson motorcycle, and finally put in an order for one. Somehow word leaked out. "Next thing I know I am receiving Harley Davidson T-shirts, very expensive ones, for months. I have quilts made out of Harley Davidson T-shirts ... the whole country just rallied.
"So do I have bad feelings about this? No! This is the best country it could ever happen to you in."
NEXT: Learn how severely wounded veterans cope when, as they struggle to rejoin daily life in this country, their fellow citizens gawk at or shun them -- and what they wish you would do instead.
Huffington Post Impact has compiled a list of organizations that seek to help veterans like the ones featured in "Beyond The Battlefield." You can read more about those groups, and ways you can help, here. Other stories in this series can be found here.