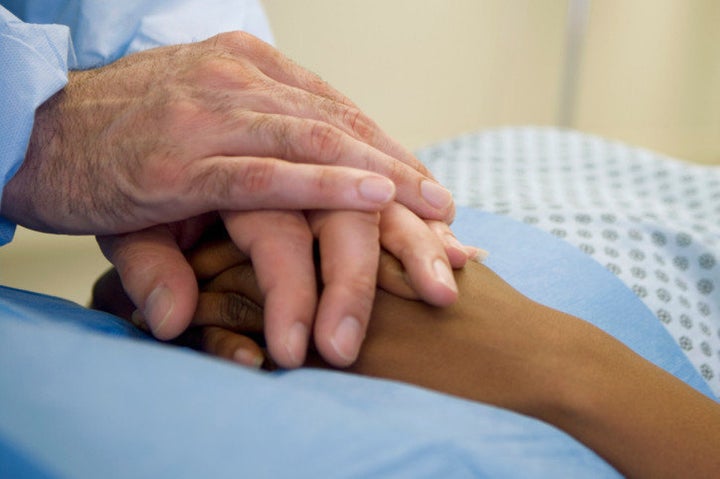
We hear a lot about the importance of compassion -- and the lack of it -- in medicine these days. Compassion comes from Latin words meaning to "suffer with." If taken literally, compassion in healing seems irrational. Why would a medical professional want to suffer alongside his or her patient? Suffering with one's patient might cloud one's professional judgment. When sick, patients need the cool-headed objectivity of their doctor and nurse -- not co-suffering or sentimentality. But compassion means more than "suffering with." It involves entering the mind-space of other persons so completely that one senses what the experience of illness is like for them.
The reason why compassion matters in healing can best be seen at the bedside. My favorite example is an event from the life of Sir William Osler (1849-1919), who is often called the "father of modern medicine." At Johns Hopkins Hospital in Baltimore, he revolutionized the teaching of medicine by bringing students out of the lecture hall for bedside clinical training, and created the first residency program for the specialty training of physicians.
After revolutionizing how medicine was taught and practiced in the United States and Canada, in 1905, at the peak of his fame, he was lured to England where he became the Regius Professor Medicine at Oxford. One day he went to a graduation ceremony at Oxford, wearing the impressive academic robes that are a feature of the occasion. On the way he stopped by the home of his friend and colleague, Ernest Mallam.
One of Mallam's young sons was desperately sick with whooping cough. The child would not respond to the ministrations of his parents or nurses and appeared to be dying. Osler loved children greatly and had a special way with them. He would often play with them, and children would invariably admit him into their world. So when Osler appeared in his dramatic ceremonial robes, the little boy was captivated. Never had he seen a human like this! After a brief examination Osler sat by the bed, peeled a peach, cut and sugared it, and fed it bit by bit to the enthralled, speechless boy. It was his first nourishment in days. Although recovery was unlikely, Osler returned for the next 40 days, each time dressed in his magnificent robes, and personally fed the child. Within a few days the tide had turned and the little boy's recovery was assured.
That's compassion. Osler had the ability to enter so fully into the mind of the little boy that he knew how to entice him to take food. He made use of the boy's imagination and wonder with his dress. He understood how to evoke a healing response in someone who was dying, all without the use of drugs or high-tech interventions. Osler was the intervention. Only someone who understands compassion is capable of such things.
Osler was noted for his ability to convey caring at the bedside of his hospital patients on brief visits. He cared greatly not only for his patients, but also for the young physicians under his tutelage. He wanted his tombstone to say only, "He brought medical students into the wards for bedside teaching." His most famous saying was, "Listen to your patient, he is telling you the diagnosis."
Some say compassion is out of date. These days, physicians have only minutes to spend with patients in most medical settings. No physician can make a house call on a single patient for 40 days in a row, as Osler did. But that is not the entire story. Compassion can be conveyed in moments; it is not proportional to time.
Compassion is not antiquated. It remains a crucial factor in healing and will never go out of style. It is always available for any healthcare professional who is wise enough to claim it.
Sources:
Bliss M. William Osler: A Life in Medicine. Oxford, UK: Oxford University Press; 2007.
Golden RL. William Osler at 150. An overview of a life. Journal of the American Medical Association . 1999; 282(23): 2252-2258.