Ever wonder how a (good) doctor comes up with her/his recommendations for treatment? What the critical thinking underlying the suggestions might be?
As an example, we can look at a comprehensive treatment plan for drug and alcohol addiction (forthcoming posts will look at other conditions, like depression, bipolar disorder and schizophrenia).
A premise I hold to is that comprehensive care should be a standard to aspire to as a patient, family member or clinician. Individual, proven treatments for a condition tend to augment one another (1+1 = >2) thereby providing a more robust response. An overreliance on one form of treatment (e.g., medications or therapy or 12-step alone), with the exception of other recognized approaches, often reflects a bias or limitation on the part of the clinician (or system of care) and seldom is in the ill person's interest.
A Substance Use Disorder (SUD) is defined as: the overuse or dependence on a drug with adverse effects on that person's physical and mental health, as well as negative consequences on others. The use of the substance, whether it is cocaine, Percodan, heroin, alcohol, marijuana or other drugs, persists despite clear and serious problems with family, work and personal relationships. Legal problems also tend to accrue.
Two related fields of science have substantially informed the treatment of a SUD -- which includes alcohol and legal and illicit drugs. These are the fields of biological and cognitive neuroscience. An understanding of the brain, still perhaps the most complex organ and system we know of, has grown vastly in recent decades. We understand far better the parts of the brain, their respective functions, their neurochemistry and circuitry, as well as how to impact them. We are far from claiming mastery of the central nervous system but that need not keep us from acting on what we know. Knowledge is what a good doctor brings to an encounter with a patient, and which should illuminate the opportunities for effective intervention.
As an example, let's consider those who are dependent upon heroin or narcotic analgesics (like Oxycontin, Percodan, and Methadone). An epidemic of their use has ravaged the U.S., accounting for more deaths than motor vehicle accidents and homicides. 12-step programs (AA, NA) have been the mainstay of intervention for SUD but today represent only one of a number of tools that can help. Comprehensive care calls for more than reliance on a 12-step program. That's where neuroscience comes in. Your doctor can offer more than AA or NA alone.
Instead of approaching addiction as a laundry list of signs and symptoms, aka conventional diagnosis, a doctor can now consider the underlying brain mechanisms driving the self-destructive behavior.
This link will take you to a psychiatric resident explaining how the brain works when addicted (it also mentions an anxiety disorder but that is extra). He uses the following drawing of the brain to describe how a treatment plan emerges from an understanding of the brain. The video is 15 minutes; the last six minutes focus on a treatment plan for a person with a narcotic addiction.
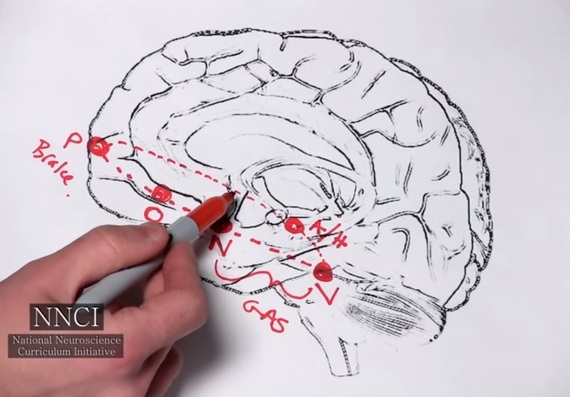
With permission from The National Neuroscience Curriculum Initiative (http://www.NNCIonline.org)
What this doctor understands -- how he thinks in developing recommendations for a patient -- is that the brain has a reward circuit that powerfully drives our behaviors. Of course, the brain is more complex but this is information for a patient and family, not a neuroscientist, and it is actionable.
Two sections of the brain (marked V & N above, the ventral tegmental area and the nucleus accumbens) signal a source of pleasure (instrumental to survival of the species - as are food and sex) by delivering a spike of dopamine. This is like an accelerator pedal. With addiction, that spike is from a narcotic not everyday life, hence the idea of how an addiction highjacks our brain from its normal sources of pleasure or reward.
The circuit then continues to the section marked O (orbital frontal cortex), which is instrumental to human drive and motivation. This region is then pumped up by the dopamine spike and gets us going, namely wanting more. It drives us to repeat the experience, even if it is a handful of narcotic pills or a needle in our arm.
But it is the P (the prefrontal cortex), where judgment and reasoning reside, that can operate to control the drive, to put some brakes on the accelerator pedal now going at a very high RPM, so to speak.
Finally, there are the A/H (amygdala and hippocampus), which are regions of the brain that store the memory of what is so rewarding. They also register what is salient to the reward; these are the cues associated with the source. Remember, Pavlov's dogs salivated, over time, to the bell not to the food, which is known as a conditioned response. It is the reward that drives us to repeat the behavior -- to survive or simply to enjoy life. But the cues offer opportunities for intervention.
In a brain addicted to narcotics this circuit of five regions is pirated because opioids (heroin and synthetic narcotics like Oxycontin and other synthetic analgesics) directly boost dopamine in the V & N sections of the brain. This triggers the circuit to powerfully fire and drives a person to seek repetitive sources of the pleasure. However, that source is not love, or food, or altruism in this case, it is finding more narcotics to ingest.
Here is where the doctor can construct a comprehensive treatment plan that targets components of the circuit, and additively increases the patient's likelihood of success:
- A number of medications are now available (Medication Assisted Treatment of Addiction, or MAT) that either block the effect of the narcotic in the V & N regions (like naltrexone) or control its release to less intense levels (like buprenorphine -- or methadone). The doctor may suggest MAT as one part of the plan.
- Motivation to resist desire to re-experience the spike -- the O region -- can be enhanced by Motivational Interviewing (MI) a brief technique that has been used in addiction for many years, and is now popular in helping people with any number of problem behaviors (e.g., overeating, tobacco use and gambling).
- The section of our brain which labors to have us use good judgment, the P region, can be substantially helped by a variety of interventions, including NA/AA, family psychoeducation and support, and promoting coping skills (like surrounding yourself with people who are not addicts, eating and sleeping well, and stress reduction practices like yoga and slow breathing).
- Finally, the A/H regions can also be impacted, especially the H region. Environmental triggers can drive cravings and relapse; these include the sight of a needle or pill, contact with other addicts or dealers, commercials about pain relief, even reports of the OD death of Philip Seymour Hoffman. Cognitive Behavioral Treatment (CBT) can be very effective in enabling a person with a SUD to avoid or have a reduced response to a trigger.
A comprehensive plan for a person with a narcotic addiction would, therefore, (with the doctor employing Motivational Interviewing) offer the patient, and supportive loved ones, a plan that included MAT, 12-step recovery, family psychoeducation, CBT, and a number of wellness activities like yoga (and yogic breathing), meditation, exercise, nutritional food, as well as the company of those dedicated to life, not addiction. This is more than a menu of services, it is recommending effective action along a variety of critical brain and behavior pathways.
If I, or a loved one, had an addiction, I would want a doctor who thinks this way. A doctor who comprehends the complexity of addiction, its neuroscience underpinnings, and the variety of treatments and self-care that, when done together, can save a person, and their family, from the catastrophic effects of untreated addiction.
Is there an argument that can be made against comprehensive treatment of this sort? Not that I know of. But it does require an informed doctor who recognizes the power of attacking tough problems in a variety of ways that augment one another. It also requires a doctor who talks with, engages, her/his patient to help them help themselves. And, of course, it takes an informed patient, family, and public to expect no less.
My thanks to Dr. Melissa Arbuckle for her groundbreaking work in teaching neuroscience.
...................
The views expressed here are entirely my own. I take no support from any pharmaceutical or device company.
Dr. Sederer's book for families who have a member with a mental illness is The Family Guide to Mental Health Care (Foreword by Glenn Close) -- is now available in paperback.
Follow Lloyd I. Sederer, MD on Twitter: http://www.twitter.com/askdrlloyd.
My website is http://www.askdrlloyd.com.