Rabies from dogs has been killing people for centuries, even millennia. It’s been that way for so long that in many countries it was just accepted that there was no practical solution.
We’ve had safe and effective vaccines that could deal with the problem for decades, but something else has changed in the last few years. Evidence has been building that the elimination of rabies from dogs is a feasible objective. Even in those areas where it was once assumed impossible there is now good evidence that the horrific deaths that rabies causes can be dramatically reduced.
Then in late 2015, rabies experts from around the globe met in Geneva and launched an ambitious vision: zero human deaths from dog-mediated rabies by 2030. They agreed that “the time is now!”, to set a goal that the global rabies community can organise behind, and that endemic countries can aspire to. As Margaret Chan, director general of the WHO said in her opening address “Rabies belongs in the history books. This event will help put it there.”

So, if we really are serious about this goal, what are our options? Most rabies endemic countries have enacted some or all of the three main approaches to preventing humans from dying:
1. Mass culling of dogs
2. Protecting people with vaccination after a dog bite (Post Exposure Prophylaxis, or PEP)
3. Mass vaccination of dogs
Time is short and money is always limited. Where do we put our money to reach this goal the fastest?
We can immediately discount the first option. Although sadly still quite common, killing piles of dogs simply doesn’t work. Time and time again a temporary reduction in the dog population is followed by the dog population rising, and rabies spreads once more. Worse still it is usually a disaster for community relations. Pet dogs are killed, guard dogs are killed, people hide their dogs or transport them away from culling teams, and this can spread rabies further afield. If there were any vaccinated dogs, these are also killed and as the population rebounds there is a fresh supply of rabies-susceptible dogs to spread the disease. After this kind of experience, the community is, with good reason, very suspicious of future rabies control attempts.
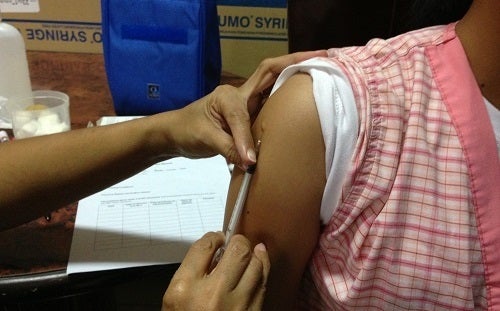
Vaccination immediately after a bite prevents rabies from developing
What about protecting people with PEP? This makes sense – we want to stop people dying, we should vaccinate them. Since only people who are bitten or scratched by a rabid animal develop the disease we can focus just on that subpopulation, which helps to reduce costs. There is no doubt that the human rabies vaccine is one of the best we have, and it saves lives – maybe 2.9 million a year. But there are practical challenges. The vaccine needs to be widely accessible and affordable, and at $40-60 for the vaccine and the health care system to deliver it to each bite patient, it is expensive for governments to provide. A lot of people get bitten by dogs – most of them were not truly exposed to rabies, but whilst rabies runs rampant through the dog population, we can’t risk waiting to see what happens before starting PEP. Rabies is almost 100% fatal and vaccination must start very soon after the bite occurs to be sure it will be effective. Huge strides have been made in making PEP available in many Asian countries, but the bills are high. In China, an estimated 15 million people are treated at a cost of nearly $650 million each year. Using human vaccination alone, these costs will continue indefinitely.

Mass Vaccination of dogs in Payatas, Manila, Philippines
So that leaves vaccinating dogs. Break the cycle of transmission in dogs, eliminate the rabies virus and everyone is protected – people, dogs, wildlife. Vaccinating dogs protects those bite victims who can access PEP and those who can’t. This method has its hurdles too of course – there are an estimated 536 million dogs in rabies endemic countries where veterinary services are generally woefully under-funded and dog health is not a priority. But it is time for some imagination – for co-operation and cost-sharing between the ministries of health that benefit from the lives saved and the ministries of agriculture or animal husbandry who could be the vital animal vaccination providers. Unlike delivering PEP which is a medical urgency, regular annual mass dog vaccination has the advantage that it can be planned ahead.
Wherever we have good animal and human data for rabies, cases in humans follow cases in animals closely. If rabies rises in animals, more people die, almost irrespective of how much PEP is supplied. A fraction of people, sometimes large and sometimes small, but always from the poorest sectors of society, still cannot access PEP. Allow me one graph, one that convinces me more than any other:
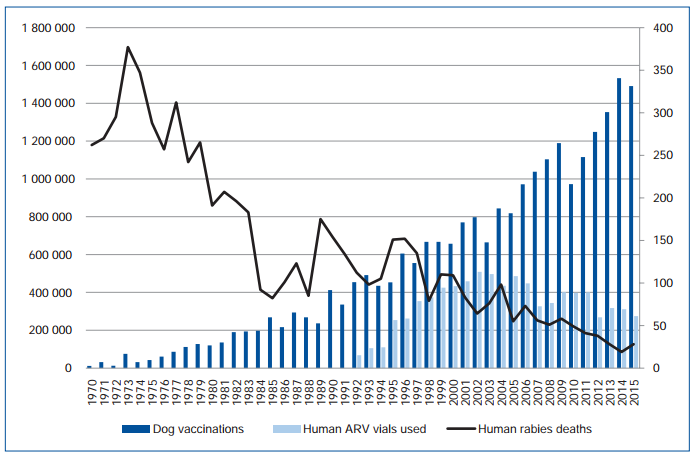
Human rabies cases and vaccination efforts in Sri Lanka
In Sri Lanka, the human rabies cases (black line) have fallen as animal vaccination (dark blue bars) has risen, and were far less affected by provision of human PEP (lighter blue bars). Rabies is an animal disease. We need PEP to protect people from the risk of rabies in the short term, but vaccinating dogs until the virus is eliminated is the only long term answer. I challenge every canine rabies endemic country to draw this graph with their own data and see what combination of efforts works best for them.
So is reaching the 2030 goal possible? Yes. We have all the tools and the know how to eliminate canine rabies for good.
Is it feasible? Yes. We have the proof of concept and the international community is ready to support countries in their efforts to build the necessary capacity.
Will it be done? That mainly depends on generating enough political will to make it a reality.
See www.endrabiesnow.org and www.rabiesalliance.org for more infomration about efforts to end deaths from rabies. #EndRabiesNow
This article is part HuffPost’s Project Zero campaign, a yearlong series on neglected tropical diseases and efforts to eliminate them. This series is supported, in part, by funding from the Bill & Melinda Gates Foundation. All content is editorially independent, with no influence or input from the foundation. If you'd like to contribute a post to the series, send an email to ProjectZero@huffingtonpost.com. And follow the conversation on social media by using the hashtag #ProjectZero.
