
BIDI BIDI, Uganda ― As far as the eye can see, tents and huts stretch into the distance.
Neck-deep in a tight trench, Jackson Wani swats away buzzing flies as he shovels soil. The stench is strong from the collapsed wall of the latrine he is shoring up, a dozen paces from his family’s makeshift home.
Wani, a 35-year-old father of three, fled from his small farm in South Sudan in 2016 when soldiers torched his village. He trekked with his family for four days on narrow forest paths to the Bidi Bidi refugee camp in neighboring Uganda.
More than a million refugees ― a population twice the size of Miami ― have arrived in Uganda since civil war broke out in South Sudan in 2013. Last year, the conflict spiraled into a man-made famine, and the United Nations warned that the situation was “fertile ground” for genocide.
The South Sudanese refugee crisis could soon be Africa’s biggest since the Rwandan genocide of 1994, and few of the displaced people hope to return home anytime soon. The Bidi Bidi camp, one of a series of refugee centers in northern Uganda, houses some 280,000 people. For several months in 2017, it was listed as the world’s largest refugee camp. No longer accepting new arrivals, it is transitioning into a settlement for long-term residents. But the flow of refugees continues into the surrounding area.
Around the world ― from regions as varied as the Middle East, Southeast Asia and Central Africa ― staggering numbers of people have fled their homes in recent years to escape war, persecution, or political instability. Over 2.6 million of them live in officially recognized refugee camps, according to the U.N.
Proper sanitation and health care are major challenges in these camps, and the diseases waiting there can be as deadly as the conflict the refugees left behind.

Tens of thousands have been killed in over four years of South Sudan’s war. But researchers who have studied conflict worldwide suggest that the number of indirect deaths could be 15 times higher than those who died in actual fighting, and disease and sickness are a core part of that. (There are no precise figures for the number of deaths in Bidi Bidi due to disease.)
At the same time, there is a pernicious misconception that when refugees flee, they bring diseases with them and sicken uninfected populations. The World Health Organization is clear that there is no systematic association between refugees and disease. Instead, the problems that refugees face are common to all who struggle in poverty.
The risk of disease increases when refugee populations are severely impoverished, like those coming from South Sudan. Many people arrived in Bidi Bidi, for example, with nothing but the clothes they had on.
“With a large number of displaced people living in close proximity, with poor water, sanitation and hygiene conditions, it leads to a risk of waterborne diseases,” said Lisa Nelson, the Uganda country director for the U.S. Centers for Disease Control and Prevention, which is supporting efforts to monitor health in the camps scattered across the forests and farmlands of northern Uganda.
For Wani’s family, like many recent refugees in Uganda, the top priority was building a shelter from fierce sun and hard rains. A family might dig out a latrine or construct a toilet much later. Many people in Bidi Bidi use communal latrines.

Aid agencies are trying to encourage households to maintain their own toilets and latrines. But it can take weeks to get new arrivals set up with a waste system that functions properly.
“We made a toilet last month, but it was destroyed in the rains,” Wani said, resting in between shoveling. “Then we dug another, but it just filled up with water. This one will be stronger, I hope.”
In this sprawling settlement, cholera, hepatitis and typhoid fever ― all associated with exposure to human fecal matter ― are big risks. With large numbers of children together, measles is also a worry. And about a third of the cases seen by camp doctors involve malaria, which is spread by mosquitoes who breed in standing water.
Wani’s 2-year-old son was sick with a fever when he spoke to HuffPost. “The doctors say it is malaria,” Wani said. “This place has so many mosquitoes about.”
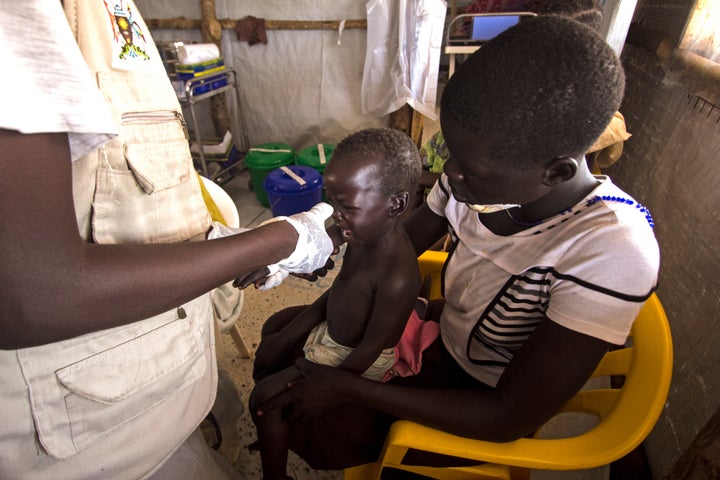
The health care system in South Sudan was already in ruins from its decades-long war of independence from Sudan, but the new nation’s civil war has made things worse. Almost all of the major neglected tropical diseases recognized by the WHO are found in South Sudan. These frequently misunderstood illnesses tend to strike the poorest, most marginalized populations with the least access to health services. They include blinding trachoma, certain types of intestinal worms, and the ferocious visceral leishmaniasis fever. In recent weeks, South Sudan has declared an outbreak of Rift Valley fever, a viral disease that can cross from animals to humans, and reported suspected cases of meningitis.
Uganda, which has a far more robust health system, has been more successful in keeping these diseases at bay. But the risk grows with the limited care and paper-thin resources in refugee camps like Bidi Bidi. Communities already weakened by war and forced from their homes are more vulnerable to disease. All crowded camps face threats of infection, although the nature of the disease changes from place to place.
For example, refugees fleeing Syria last year struggled with an outbreak of cutaneous leishmaniasis, a parasitic disease spread by sandflies that causes boils and lesions.
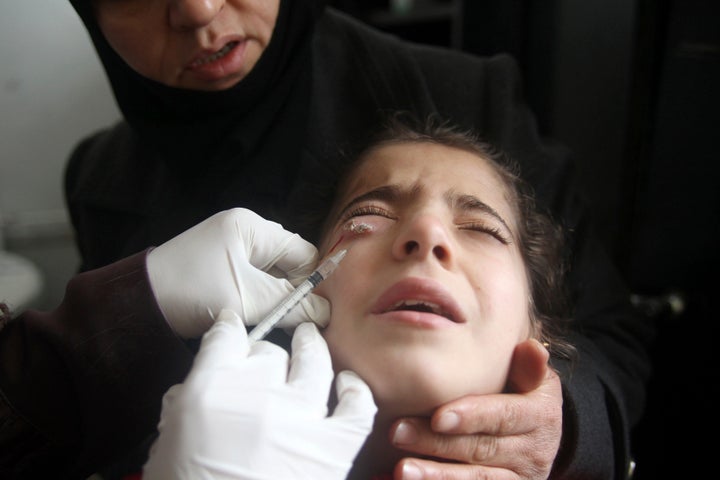
“A refugee camp is a hotbed for disease,” said virologist Dr. Julius Lutwama, deputy head of the Uganda Virus Research Institute, a government-backed center that tracks disease. “Congregation is one of the biggest problems for transmission.”
Soon after the South Sudanese refugees arrived, the Ugandan government handed out plots of land to each family in Bidi Bidi and the surrounding camps. The scrubland was enough to build a small hut and carve out a patch to plant crops.
But there was a reason the land here was sparsely populated. When the rainy season comes, some areas turn into bogs.

Water and sanitation experts are trying to help the people who live in these settlements. Red Cross volunteers advise on the best way to construct latrines to withstand Uganda’s heavy rainy season and offer practical guides to installing handwashing stations and digging pits for trash. Yet overstretched doctors can barely cope with the flood of patients who come in every day.
Dr. Ogwal Daniel, working for the International Rescue Committee, runs the largest clinic in the Palabek camp, which unlike nearby Bidi Bidi is still expanding with new refugees. The one doctor and a team of nurses see over 100 patients each day.
“You have to make do with what you have,” Daniel said, waving at his clinic, a wooden frame with plastic sheeting for the roof and walls. On the other side of the flimsy structure, a baby with a malaria fever wails as a nurse slides a needle into his arm.
“Of course, we could always use more, but we adjust to the situation,” Daniel said.
This article is part of HuffPost’s Project Zero campaign, a series on neglected tropical diseases and efforts to fight them.

