PART 2
Following in this second installment of a three-part special series delving into the challenges of living with sickle cell disease is a story focusing particularly on the pharmaceutical and genetic developments being pursued to help overcome these challenges.
Talk to a sampling of those well entrenched within the sickle cell community, and the prevailing sentiment that echoes is, yes, there’s still a ways to go to bring lasting relief to the individuals afflicted with this disease. Or even greater awareness of the consequent physical, economic, social and emotional complexities that permeate their lives.
Yet the likelihood of better days ahead in the foreseeable future seems more certain than ever.
After all, researchers have come to understand a lot more about the precise genetic mutation that causes sickle cell disease. More so than when they first began to realize its hereditary nature, and molecular treachery, in the 1950s.
Or, in the 1970s, just how the abnormal hemoglobin that people with this disease are born with causes their red blood cells to, at times, morph into stiff, sickled shapes that clump together and clog the smallest vessels throughout the body. Pair that with the onset of better screening for sickle cell disease back then; and, thanks to the Civil Rights Movement, unified push for more funding and research of this disorder with a prevalence of black sufferers.
Much improved preventative drug treatment and medical care, and even more aggressive research in the ensuing decades have toppled sickle cell disease as the overwhelming childhood death sentence it once was. These days, half of all patients in middle- to high-income countries reportedly live past age 50.
“In 2016, when I see a newborn with sickle cell disease, I can tell the parent that there is greater than a 98 percent chance of [his or her] child reaching adulthood,” affirms Dr. Michael R. DeBaun. Tremendous odds considering there’s only one prescription drug available to those of any age with sickle cell disease to counteract their illness, notes the director of the Vanderbilt-Meharry-Matthew Walker Center of Excellence in Sickle Cell Disease, in Nashville, Tenn.
And even that limited offering is merely in affluent nations like the U.S., where the Food and Drug Administration (FDA) finally approved the lone sickle-cell drug accessible in this country, longtime chemotherapy medication, hydroxyurea, back in 1998. Nearly a century after sickle cell disease was first identified, bear in mind.
“A single drug for such a serious medical condition is woefully inadequate,” charges Dr. Alexis Thompson, a pediatrics professor in Chicago at Northwestern University’s Feinberg School of Medicine.
The lag in development does appear to be shifting, however. Dramatically.
“These are very exciting times for the sickle cell community.”
—Dr. Alexis Thompson
A pharmaceutical company is awaiting FDA approval at this very moment to introduce a second commercial drug that, by actually preventing sickle cell symptoms as well, could improve the quality of life for its sufferers considerably. Two other companies are set to begin their third and final clinical phases of evaluating such drugs. While yet another company is planning to launch a Phase I trial next year of a gene-editing technique to actually cure sickle cell disease.
“These are very exciting times for the sickle cell community,” grants Thompson. “Advances in our understanding of basic mechanisms underlying this disease have occurred over decades, but the translation of these discoveries into potential treatments seems to be accelerating right now.”
For the time being, however, people with sickle cell disease must continue to make do with therapeutic measures that help ease, but don’t eliminate their pain and suffering.
Current remedies to deal with the physical pain that can rack their arms, legs, chest, stomach, lower back, and joints and bones range from heating pads, hydration, massages and over-the-counter medicines like aspirin and ibuprofen, to morphine and other prescribed narcotics.
The downside to hydroxyurea is that some people can’t tolerate the weakened immune system and other side effects that can come from taking it. While Jadenu tablets, the latest prescription drug available to people with sickle cell disease, only combat the chronic iron overload that can come from the routine blood transfusions that doctors employ to prevent strokes and other complications in such patients.
Still, these small oval tablets manufactured by Swiss pharmaceutical giant Novartis AG and FDA approved last year are said to be the only daily oral medication that can be swallowed whole, with or without food, to treat such setbacks. Earlier medication for iron overload had to be dissolved in liquid and drank on an empty stomach.xdc
STEADY ADVANCES
Not to be left out of the quest to develop new and improved drugs for sickle cell patients, Pfizer Inc. is seeking at least 350 such individuals, ages 6 and older, in which to test one called rivipansel.
Administered intravenously, rivipansel is intended to stop the inflammation and adhesion of red cells to the lining of blood vessels that send children and adults to the hospital in sickle-cell pain crises. So far, the FDA has not only granted rivipansel the orphan-drug status that nations allot to select experimental treatments of rare and genetic health conditions. But also its Fast Track designation to get critical medications on the market as soon as possible.
Pfizer has paid $35 million to the originator of rivipansel, Gaithersburg, Md., novice GlycoMimetics Inc., since 2011 in a worldwide licensing agreement to develop and commercialize this trial medication. Now the New York-based pharmaceutical behemoth is targeting the second half of 2018 to finish its current recruitment of patients hospitalized during a sickle cell pain crisis that will facilitate a Phase III clinical evaluation of this drug.
“However, this is dependent on the rate of enrollment in this trial,” says Dr. Kevin Williams, chief medical officer of rare diseases in Pfizer’s Innovative Health division. “Patient enrollment in clinical trials, which is a challenge in many therapeutic areas, can be particularly challenging in rare diseases.”
“Over the years, a number of new therapies have been tested by different companies,” Williams, an internist by profession, elaborates.
“Some have failed because they weren’t safe enough or effective enough,” he continues. “But more than half have failed because the developer of the medicine wasn’t able to recruit enough patients to complete the clinical trials to evaluate whether the medicine was safe and effective.”
“Participation in clinical trials is vital,” says Williams. “Those who join clinical trials are the heroes — unsung heroes, really — of biomedical progress. Without them, progress simply would not be made.”
With FDA Fast Track and orphan-drug endorsement as well, Global Blood Therapeutics Inc. will need such heroes for the final phase of investigating its GBT440 that that the company is now gearing up for.
Taken once a day, for life, this pill is intended to prevent red blood cells from sickling not only in adults susceptible to this defect, according to the San Francisco developer of pharmaceuticals for severe blood disorders. But in adolescents as well, if the company’s ongoing studies are any indication.
Dr. Eleanor L. Ramos, chief medical officer for Global Blood Therapeutics, explains that hemoglobin molecules normally “exist as single, isolated units in the red blood cells.” But for people with sickle cell disease, she goes on, these molecules can “stick together, or polymerize, when they release oxygen in the (body’s) tissues,” which is what causes the red blood cells they occupy to sickle and prematurely break down.
GBT440 works by causing oxygen to bind much tighter to hemoglobin during normal blood flow, explains Ramos. An upshot that Global Blood Therapeutics reported throughout the summer proved not only to prevent red blood cells from losing oxygen abnormally and prematurely. But, in turn, sickling and dying out early as a result.
Now the company is looking to meet “with U.S. and European regulatory authorities to define the future development plan for GBT440 with the goal of initiating a pivotal Phase III trial” before this year is up, Ramos discloses.
“Those who join clinical trials are the heroes – unsung heroes, really – of biomedical progress.”
—Dr. Kevin Williams
Leading the pack of pharmaceutical companies vying to bring new prescription sickle-cell drugs to market is Emmaus Life Sciences Inc. Having completed an FDA priority review process that it began after finishing a Phase III clinical trial in 2014, the Torrance, Calif.-based company is now formally appealing to the FDA to approve its L-glutamine capsule for commercial use. L-glutamine is an antioxidant-producing amino acid found naturally and abundantly in the body that scientists have discovered offers a powerful defense against the output of red blood cells that get sticky and block small vessels.
The recent move by Emmaus Life Sciences to get the FDA to sign off on commercial use of its L-glutamine offering came strategically — amid the National Sickle Cell Awareness Month observed in September. And after more than 20 years of research invested in a daily oral regimen that, FDA-authorized for Fast Track development and orphan-drug usage in the U.S. and Europe, has become the company’s foremost potential offensive against sickle cell disease.
As this impetus to get advanced drugs to those with the disease proliferates, some researchers remain hopeful about what hydroxyurea can do to alleviate the suffering of children who have this genetic disorder. The medicine has already helped to reduce hospital admissions, blood transfusions and a serious condition resembling pneumonia known as acute chest syndrome for adults with sickle cell disease since being FDA approved to treat them nearly two decades ago.
Taken once a day as a liquid or capsule, hydroxyurea works by stimulating the production of fetal hemoglobin — rife in newborns — to inhibit the formation of red blood cells that sickle. The ability of fetal hemoglobin to retain oxygen long enough to be aptly supplied to all of the body’s tissues is what suppresses this mutation.
“In the last five years, there has been a surge in the number of Centers of Excellence at hospitals in large cities,” says Michael Higgins, a senior research analyst in the New York office of ROTH Capital Partners LLC who tracks the pharmaceutical industry. “At these hospitals, it’s common to see 60 percent of sickle cell patients on hydroxyurea, as these hospitals aggressively address the side effects [of this disease].”
For Shaletha Booth, getting her daughter, Kynnedi, included in a federal study of babies on hydroxyurea before the child’s second birthday has been their best medical defense yet against sickle cell disease.
“This medication has helped her tremendously,” says Booth. “When she started on it she went, like, a year or two with no problems.”
Now, at 10 years old, “I would say she has maybe had six bad crises,” Booth goes on about the daughter she learned had sickle cell disease two weeks after giving birth to her. “For her to have the most severe case, which is [hemoglobin] SS, and not have a lot more problems, at one point I was like, they must have diagnosed her wrong.”

Kynnedi Jones approaching tweendom.

Kynnedi's grandparents, Linda and Eddie Booth, started a sickle cell awareness walk in Flint, Mich., during the summer of 2014.
Unfortunately, the diagnosis was not wrong. To the contrary, it was a pronouncement that brought the reality of sickle cell disease home for the 32-year-old pharmaceutical chemist like never before.
Now living along the Eastern Shore of the U.S., in Salisbury, Md., with Kynnedi and another 3-year-old daughter, Booth says that she has known she carries the genetic trait for this disease since growing up in Flint, Mich. And her parents, who launched a walk in her hometown two summers ago to help raise awareness about sickle cell disease, were diligent to caution her about having children with another carrier.
After all, Booth has a sibling with sickle cell disease. That’s a one-in-four possibility for any couple like her father and his first wife, who both carry the genetic trait for the illness. But being 18 years her senior, Booth notes of her half brother, he didn’t grow up with her, minimizing her first-hand experience with sickle cell disease.
Then there’s the insidious habit that being young and in love has of clouding judgment and foresight. Booth says she never considered that a friend of her older sister who she began dating as a biology major at Alabama A&M University might carry the sickle cell trait. Even though one in 12 blacks in the U.S. is, like her, a carrier, she concedes that the subject never came up in their relationship until she got pregnant.
“We were together for three or four years before we had her,” Booth divulges about her eldest daughter’s father. “I guess that’s one of the questions that I never thought to ask him. I didn’t really have a reason to ask. We were always very serious and I always thought I was going to marry him.”
But being asked at her doctor’s office about his sickle cell status after learning she was expecting was an eye-opener. When Booth later finally did ask him if he had the trait and he answered yes, she recounts, “That’s when it hit me that this could be a problem.”
“You know how people always ask you, ‘What are you having, a boy or a girl?’” Booth, who says terminating her pregnancy was never a possibility she considered, tearfully reveals about that time of her life. “My response would always be, ‘I just want to have a healthy baby.’”
After her daughter was born, the first sign that something might be amiss with Kynnedi’s health came when it was time to feed her. According to her mother, she just couldn’t keep down the different brands of infant formula that Booth tried to alternate with nursing her. When Booth turned to Kynnedi’s pediatrician at the time to get to the bottom of what was going on, the feeding problem took a back seat to being told what no parent wants to hear. Ever.
Her child had come into the world with a lifelong, incurable illness. One that she and Kynnedi’s father had passed along to their daughter.
Kynnedi was immediately put on a daily regimen of penicillin after her sickle-cell diagnosis. That was to reduce her risk for the severe infections that often killed babies with her disease before doctors regularly began prescribing them this antibiotic in the late 1980s.
As babies with sickle cell disease don’t usually show symptoms until after 6 months of age, Kynnedi didn’t until she was about 14 months, when the ring finger on her left hand became noticeably tight and swollen one day, Booth recalls. She had her first major crisis four months later, when her left leg started to swell.
“They actually had to go in and cut her leg to relieve some of the swelling,” says Booth “She still has the scar on her left leg. Then they had to put a C-line in her chest, and out the neck.”
Booth still remembers the long syringe she continued to give her daughter medicine with at home, once a day for the next six weeks via the soft, plastic intravenous catheter known as the central line (or C-line).
“I had a nurse who taught me how to do it,” she says. “When she went to daycare I covered it with gauze. The nurse would travel to daycare to get her blood work.”
All the while, Booth says she constantly researched sickle cell disease on the internet. Which is how she learned about the Pediatric Hydroxyurea Phase III Clinical Trial, better known as the BABY HUG study, just before Kynnedi turned 2. This was a six-year undertaking in the U.S. by the National Institutes of Health to analyze the potential benefits of hydroxyurea to 9- to 18-month-old babies who either had hemoglobin SS, like Kynnedi, or another form of sickle cell disease called sickle beta-zero thalassemia.
Funded specifically by the National Heart, Lung, and Blood Institute, and the National Institute of Child Health and Human Development between October 2003 and September 2009, nearly 200 babies nationwide were each given 20 milligrams a day for two years of liquid hydroxyurea. Or, unbeknownst to either the parents or researchers until the end of the study, a placebo instead.
Aided by Dr. Thomas Howard, a pediatric hematologist/oncologist in Birmingham, Ala., that Booth had started taking Kynnedi to, she was able to get her daughter enrolled in BABY HUG at about 15 months old. And for the next two years drove three hours round trip, once a month, from where she lived in Huntsville, Ala., to Children’s of Alabama, the Birmingham hospital where Kynnedi participated in the study.
After that, Booth opted to allow her then nearly 4-year-old to continue undergoing periodic blood tests and and other clinical evaluations as Kynnedi explicitly took hydroxyurea. Having started on the liquid form of this medication, the child now takes capsules.
“Kynnedi does phenomenal,” Booth sums up of the tiny, soft-spoken girl that, she shares, loves computer and video games. “She does have her problems here and there. As she gets older, I do notice that her eyes get jaundiced. In school, [when she was younger] she caught on to things super quick. Now that’s she a little older I do notice that she doesn’t catch on to things as quickly as I would like, but she does catch on.”
ON THE HORIZON
Beyond the glimmers of hope that pharmaceutical advances like hydroxyurea seem to have cast in families like Kynnedi’s, researchers are also delving into the genetic origins of sickle cell disease to find ways to reverse it completely. Especially via tentative yet scientifically enticing procedures to, literally, tweak the genetic makeup of sickle cell patients with infusions of new or altered stem cells that prompt their bodies to generate only healthy red blood cells.
At present, that primarily means gene therapy. Or, to be more specific, implanting stem cells extracted from the bone marrow of a sickle cell patient with ostensibly harmless engineered viruses containing a new gene that counteracts the deviant hemoglobin at the root of this disease. The modified stem cells are then put back into the patient, thus allowing his or her body to then, make hemoglobin that forms normal pliable, doughnut-shaped red blood cells.
Last month, researchers at the Dana-Farber/Boston Children’s Cancer and Blood Disorders Center reported that the precision-engineered gene therapy virus they developed and injected into blood stem cells, then transplanted, significantly decreased sickle-induced, red-cell damage in mice with sickle cell disease. Encouraged by these preclinical results, this team of researchers is now petitioning the FDA to begin clinical studies on humans next year.
Their peers at the University of California, Los Angeles have been conducting such trials for the past two years within the university’s Eli & Edythe Broad Center of Regenerative Medicine & Stem Cell Research. Also at the forefront of pursuing this biomedical approach to curing people of sickle cell disease are researchers at the likes of the Massachusetts Institute of Technology, John Hopkins University, Harvard University, Stanford University and the University of California, Berkeley.
Researchers at bluebird bio Inc. in Cambridge, Mass., are conducting a Phase I trial of a virus-based drug to remedy the genetic mutation that causes a person’s red blood cells to sickle called LentiGlobin BB305. Remedy that, and thalassemia (or Cooley’s anemia, for Dr. Thomas Cooley, the pediatrician who first described this particular hemoglobin disorder in 1925). The FDA has granted the use of LentiGlobin BB305, for either condition, the Breakthrough Therapy designation that it also offers to help expedite drug development for serious or life-threatening diseases.
In the meantime, a teenager in France was able to stop getting blood transfusions altogether, without any subsequent complications, after becoming the first sickle-cell patient to undergo treatment with LentiGlobin BB3305 last year.
Couple such an outcome with how gene therapies don’t pose the risks and challenges of the cell therapies now chiefly used to fend off the destruction of sickle cell disease. Like the iron overload from repeated blood transfusions that can damage a person’s heart, liver, pancreas and other organs. Or, in the case of bone marrow transplants — the only sickle-cell cure now publicly, albeit sparsely available — the chemotherapy needed to destroy a patient’s bone marrow (and, thus, immune system) so as not to reject marrow-producing stem cells from a donor. Or even the harrowing need to find a donor in the first place.
No wonder so many startup companies have been able to raise what The Boston Consulting Group estimates is more than $1 billion within the past two years to advance gene editing.
The financial backing has come for this even more intricate method of biological manipulation to eradicate sickle cell and other genetically based diseases, despite the fact that no human genetic engineering of any kind has been approved commercially in this country. Or elsewhere, yet.
Undaunted, scientists at these startups remain busy cultivating the means to directly modify the genes of fully developed, living organisms — up to and including humans — in research labs from Seattle to Boston to Switzerland, Germany and beyond. Without the procedural limitations, moreover, of genetic engineering in decades past that only let their predecessors insert foreign DNA into cells at random.
A foray that, in some cases, led to such life-prolonging inventions as the synthetic insulin formulated from E. coli bacteria mixed with a human gene that’s now used by millions of diabetics worldwide to control their blood sugar levels. And unfortunately, in other cases, stimulated cancer-causing genes and other health catastrophes in people seeking escape from a life of illness.
Take the two children in France who were cured of the rare “bubble boy” immune disorder in 2003 by the very gene therapy that later spawned leukemia in them. Both survived with treatment, but not every patient has been as fortunate.
Jesse Gelsinger is a tragic example of that. Just 18, the Tucson, Ariz., high school graduate elected to undergo an experimental gene therapy at the University of Pennsylvania in September 1999 to cure his mild form of a rare metabolic disorder. Instead, four days after the procedure he was brain dead, with jaundice, massive blood clots, and liver and kidney failure having first besieged his body.
Yet such tragedies don’t seem to be enough to sway the growing fervor among scientific circles for the possibilities of genetic engineering. Especially with endorsements from the likes of the head of the FDA.
In the keynote address at the University of Miami’s clinical trials conference last month, Dr. Robert M. Califf, commissioner for the agency, shared that four years ago he would have deemed the notion of scientists merely replacing disease-causing genes with healthy ones as science fiction.
“But it turns out that we now have technologies that can do this,” granted Califf, a cardiologist by profession. “We’ve gone from looking at the downstream products of what genes do and using genes to make a diagnosis, to actually being able to go in and to either delete a gene, insert a new gene in place of a gene that was there, or add a gene to the genome — and doing it very specifically with little molecular scissors.”
Similar to how a writer can edit text on a computer, scientists have indeed happened on the potential to surgically implant, replace or, with these artificially contrived “molecular scissors” snip away at DNA to correct the genetic flaws that make people incurably sick. And not only with unprecedented speed and accuracy, they tout. But far more affordably than older gene-editing mechanisms as well, thanks to a discovery given the acronym CRISPR/Cas9 by scientists at UC Berkeley in 2012.
Pronounced “crisper,” CRISPR stands for “clustered regularly interspaced short palindromic repeats,” which are the unusual, recurring DNA sequences that Japanese scientists first noticed in E. coli as far back as the late 1980s. In time, the scientific community came to realize that these sequences are part of the natural immune system within bacteria to help these microbes fight off invading genetic materials.
Just as our immune system remembers the pathogens it has fought, these sequences give bacteria a physical record of the viruses they have encountered. Should these viruses return, a set of “CRISPR-associated proteins,” the best known being the Cas9 ones that come from strep throat-causing bacteria, is dispatched to locate them, via a guide of RNA molecules, and slice them up.
This groundbreaking capacity to restructure the genetic makeup of live organisms has catapulted the biomedical world into a research frenzy to harness such potential for cures to sickle cell and other diseases caused by a single genetic mutation. And, in time, to more complex illnesses involving multiple genes as well, like cancer, diabetes, heart disease and certain neurological disorders.
Vertex Pharmaceuticals Inc. of Boston. Juno Therapeutics Inc. of Seattle.
Caribou Biosciences Inc. of Berkeley, Calif. Cambridge-based Editas Medicine Inc., and Intellia Therapeutics Inc.
Crispr Therapeutics AG of Basel, Switzerland.
These are but some of the new research companies that have been spawned from the promise of CRISPR/Cas9. While global pharmaceutical corporations such as Novartis and Germany’s Bayer AG get in on this gene-editing craze partnering with the likes of Caribou Biosciences and Intellia Therapeutics.
“The application possibilities are beyond imagination,” say Elsy Boglioli, a partner and managing director with The Boston Consulting Group, and her colleague in the Paris office of this global firm, project leader Magali Richard.
“Once a fully dedicated research subject, gene editing is becoming a routine manipulation in life science laboratories,” they assess in their September 2015 commentary, “Rewriting the Book of Life: A New Era in Precision Gene Editing.”
In fact, Editas Medicine plans to begin a Phase I trial of its gene-editing technology next year, discloses company spokesperson Tim Hunt.
But such prospects for tinkering with humankind have not come about without a morass of challenges to sort through.
Like the patent war over the CRISPR gene-editing technology now waging between two of the most formidable centers of research and higher learning in the U.S., UC Berkeley, and the Eli and Edythe L. Broad Institute of MIT and Harvard. Or all the ethical quandaries that loom with being able to manipulate genes so easily, from the possible ecologic mayhem of unleashing inadvertent mutations among the plant and animal kingdoms, to conceiving species-targeting bioweapons and, yes, designer babies.
“…as history has shown us, any technology is but a double edged sword,” Ulson Gunnar, a New York-based geopolitical analyst and writer, cautions about human gene editing in the June 5, 2015, issue of the online magazine, New Eastern Outlook. “Whatever good it is capable of, it is proportionally capable of just as much bad.”
For now, the scientific consensus is that reconfiguring the genetic makeup of any one person, let alone among the human masses, is still years away. And, thus, any medical cures that might come from that.
DAY TO DAY
The Sant family doesn’t have that kind of time.
The eldest child in this brood of five living in Winston Salem, N.C., has been receiving blood transfusions at least once a month for the past two years to keep the sickle cell disease that has ravaged his 8-year old body from killing him. But his parents, Lucas and Aline Sant, are ever mindful that while these transfusions may be prolonging their son Caesar’s life for now, they ultimately could, in fact, jeopardize his life.
“The transfusions mitigate the strokes,” three in two years that the boy has already endured, his father, Lucas Sant, pointed out over breakfast at home one morning with his wife and all three children. “But over time there are side effects. The liver, eyes, kidneys and other organs are compromised.”
As such, Sant and his wife are desperate to get Caesar the bone marrow transplant they’re convinced will make him better once and for all. Also known as a stem cell transplant for the stem cells that produce normal blood cells contained in the marrow of a healthy donor, such transplants are mostly done for children with severe sickle cell disease. Although 36-year-old Chicago mother Ieshea Thomas was the first Midwest sickle-cell patient to undergo this procedure successfully, without the initial preparation of chemotherapy, at the University of Illinois Hospital & Health Sciences System in 2012.
Still, with children, their youth tends to make them less likely to have the organ damage that adults can suffer from this disease over time. And give them more stamina for an aggressive treatment that typically requires high doses of chemotherapy to destroy all their bone marrow so as to make way for a donor’s marrow. Plus, immunosuppressants that, taken for months to years afterwards, can cause serious side effects.
“He cannot stay too much longer on the blood transfusions,” Sant concedes of his son, a violin prodigy who was left completely paralyzed and unable to speak after the last of the strokes that he began having at age 4. “It’s just a matter of getting the money.”
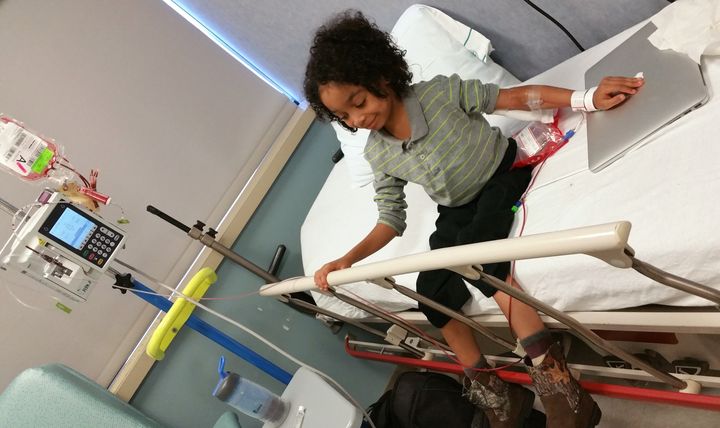
Caesar Sant undergoing a blood transfusion.
About half a million dollars, he and his wife anticipate. An amount all the more daunting to come up with in light of the fact that Sant, a 20-year neuroscientist, left his job at Wake Forest University in June 2014 to take care of Caesar fulltime. His wife, who parlayed an undergraduate law degree into working for Brazil’s federal revenue department before migrating to the U.S. with her husband nine years ago, has been a stay-at-home mom ever since.
“Even when I went to work, I was there but my head was not there,” Sant explains of his decision. “My wife was five months pregnant with Helen (their youngest child) and my son was not able to do anything, not even hold a pencil.”
Generating some income these days from the research papers he gets published, Sant’s health insurance ran out in July 2015, ending the formal physical therapy that Caesar had been receiving.
“We adjusted the house to work with him,” says Sant, who continues his son’s rehabilitation himself at home. “I learned from his physical therapist and use my common sense, so it helps. We’re doing quite well with that.”
Caesar has, in fact, regained about 90 percent of his body’s mobility, according to his parents, and is back to being his typical bright, energetic self. Home-schooled, he has regained the ability to write that his temporary paralysis stunted, they detail, and is tackling math and reading a year ahead of his grade level as well. When he isn’t singing constantly, that is, sometimes for an hour at a time, at full volume, with his two little sisters.
Caesar is even playing the instrument again that he has amazed both music teachers and audiences with since the age of two, his parents say of a little boy who also can speak six languages.
“Every day we laugh and cry,” Sant shares. “After the last stroke, I actually had a doctor tell me Caesar wouldn’t survive. I always tell people you have to have faith. I do have faith. It’s not big; it’s a little bit. But I told my wife, I told myself, I told Caesar I will give my life to you. That is what I do.”
So far, that has included emptying his 401(k) to help cover his son’s medical expenses. And spearheading two fundraisers through Go Fund Me and the national, nonprofit Bone Marrow Foundation. The generosity of friends has been a financial godsend to the Sant family as well.
“Friends say, ‘Lucas, I don’t have much but here, here’s $1,000’,” cites Sant. “One friend donated more than $50,000.”
Sant and his wife now hope to have Caesar appear on PBS and other television venues like the “Oprah Winfrey” and “Ellen DeGeneres” shows in order to generate more exposure and, thus, more money for their son’s plight. In the meantime, NBC’s “Today” show recently shot footage of their son that the morning program plans to feature soon, according to Sant, while National Geographic is planning an update of a video special on the boy that it aired last year.
The Sants already have their ideal donor for Caesar once they have enough money to get him a bone marrow transplant: his youngest sister, 22-month-old Helen.
Caesar’s other sister, 6-year-old Maria-Anita, can’t donate because she, too, has sickle cell disease, though she has only exhibited it once, their mother notes, when an incident at 7 months old required her to be hospitalized. While doctors are working on being able to cure sickle-cell patients with bone marrow from healthy non-related donors, for now, the best match has proven to be a sibling without the disease.
That’s why Lucas and Aline Sant turned to in vitro fertilization to conceive Helen. And the couple was able to have three times more stem cells collected from the umbilical cord blood that Helen was born with, in storage ever since, than what Caesar is expected to need, notes Lucas Sant.
“She doesn’t have sickle cell and she 100 percent genetically matches Caesar,” says Aline Sant. “Now she’s the life of our family.”
“All I need is for Caesar to get this transplant,” continues Aline, who shares that she wasn’t even aware that she carried a trait for a disease that could be passed on to her children until she was pregnant with Caesar. Before 2002, when all newborns in Brazil began to be tested for sickle cell disease, she explains, people only were tested there if they donated blood, which is how her husband learned years ago that he had the trait.
“It’s scary,” Aline divulges of having a child who never displayed any symptoms of the disease until he was 4 years old. “You are [constantly] learning about something that your child has that, even though they’re fine one minute, they can have something happen in the next minute.”
What scares Tosin Ola-Weissmann is the thought of not being around to finish raising her 21-month-old twins, Ariel and Orion.
“The CDC (Centers for Disease Control and Prevention) puts the mortality rate for women in the U.S. with sickle cell disease at 42 to 45, and I’m 36,” acknowledges this first-time mom. “That’s terrifying for me. My boys will only be 11 years old. I don’t want them to live their lives without their mother.”
A registered nurse living in suburban San Diego with her sons and husband of nine years, Ola-Weismann has instituted a daily regimen of juicing fruits and vegetables and taking hydroxyurea in an urgent bid to improve her chances of survival. Instituted that, and trying to avoid a leading instigator of sickle cell pain crises – stress – as best she can.

Tosin Ola-Weissmann and her family.
But Ola-Weissmann is up against a disease that has inflicted even more havoc on her body since having children.
“Before the babies, I would have a crisis about every other month, so about six times a year,” she shares, likening the agony of these episodes to three times that of being in labor. “Now I have an excruciating pain crisis every month, sometimes even up to three a month.”
“I think getting pregnant depleted all my reserves, and I’m having more pain in my right leg,” continues Ola-Wesismann. “I also have avascular necrosis of the hip. The sickled cells tend to clump whenever they’re feeling stressed and finicky, and can cause clotting. The clots cut off circulation and cause that area of the bone to die. Every time I walk, it’s like bone on bone. That comes with its own pain. Eventually, I’m going to require hip replacement surgery.”
Determined to persevere nonetheless, Ola-Weissmann says that she’s considering her hematologist’s recommendation to become part of a blood-exchange infusion program. Meaning she would be infused with 8 units of blood new to her body every month, for the rest of her life, she explains.
“I haven’t decided to do it yet because it’s already difficult for them to match my blood when I have a crisis and go to the ER,” reasons Ola-Weissmann. Just with the 2 units once or twice a year that she’s given at most now whenever her blood levels get so low during those times that she winds up hospitalized.
“Essentially, the blood I was born with is not the blood I have now,” she adds. And, as a result, is laden with antibodies against specific blood types that have developed from her multiple transfusions. In turn, making it that much harder to find compatible donors and putting her at greater risk for potentially deadly reactions and infections with future blood exchanges.
“The transfusions are a band-aid,” Ola-Weissmann concedes of her genetic propensity for episodes of agonizing pain that, in addition to stress, can be brought on by dehydration, flying, menstruation, lack of sleep, or sudden exposure to drastic temperature changes. “It’s not a long-term solution. My bone marrow is still producing sickled red blood cells.”
As such, Ola-Weissmann continues to live day to day with the threat of what something even as ordinarily benign as sharing affection with loved ones can do to her. Like the time she kissed her husband while he had a cold, contracted the infection that was making him sick, and wound up hospitalized.
Yet she endures not only on whatever temporary physical relief that existing medical treatments now avail her. Or the sheer will as well to stay alive for a family that now includes two baby boys with the trait for the very disease she has fought her entire life. (An unfortunate inheritance from Ola-Weissmann, as her husband doesn’t have the sickle cell disease or trait.)
Further motivating Ola-Weissmann in her quest for longevity is Sickle Cell Warriors Inc., the nearly 17,000-member strong nonprofit advocacy and education group that she launched as just a blog while hospitalized from a sickle cell crisis 10 years ago. And the possibility of a far better quality of life, if not a cure, offered by new drugs being developed.
“There are several treatments that look promising,” says Ola-Weismann. “For me, I’m fine living with sickle cell disease. I just want there to be more treatment options to where if I go to the ER while I’m going through a crisis, I don’t want them to just give me pain meds. That doesn’t fix the problem. It’s not helping my blood. It’s not helping my tissues. It’s not helping my organs.”
Next in the final story of this series is an examination of the racial thicket that has long entangled the sickle cell community in stigmatization and inequalities in health care and research. Go here to access all of the stories. The author, King, is a writer, independent filmmaker and actress in Metro Detroit. A carrier of the sickle cell trait, she was inspired to write this special series by the loss of three sons, ages 5, 31 and 50, to the actual disease within two years in families she knows or knows of. To learn more about King, visit A Square Peg/Round Hole Creation, LLC.
