
A diorama about a military sexual assault, where the figure in pink is the victim (male, female or transgender) and the green figures are the assailants. The staging of the figures was part of an impromptu discussion with noted MST advocate, Susan Avila-Smith.
To the extent that conversations about military sexual trauma, at least online, shed little light and often a fair amount of heat, it seems wise to create some sort of primer about what military sexual trauma is and isn’t, who it happens to, and a few other crucial factors.
The cumbersome phrasing, “Military Sexual Trauma” (MST), is codified wording in use by both the U.S. Department of Defense (DoD) and the U.S. Department of Veterans Affairs (VA). At its core, it refers to the entire spectrum of incidents from sexual harassment through sexual assault and rape, including gang rape, that happens in the military. It’s important to note that it isn’t its own diagnosis, per se, with VA; so veterans who disclose to VA that they are MST survivors — and VA screens for that — have it noted in their medical charts but the actual diagnosis is for what MST leads to, for example, frequently Post-Traumatic Stress Disorder (PTSD). Confused already? We understand.
(For the uninitiated, the Department of Defense is the relevant agency while a service member is on active duty or in the guard or reserve. When a service member leaves their military service — “separates,” in the actual lingo — they become a veteran and their primary connection is now with VA, for an array of services, although not all veterans choose to enroll or utilize VA services. Additionally, reservists are not eligible for VA services, which is why they see primary health care providers in their community for diagnosis and treatment. However, fortunately, guard and reservists who have experienced MST are eligible for VA treatment, as is clarified in this fact sheet.)
While technically MST takes place while someone (male, female or transgender) is serving in the military, researchers like RAND typically ask whether the incident took place during the past year, or over the course of the respondent’s military service. (The percentages are obviously quite different.)
To compound the problem, there are various reasons why service members in particular — although veterans as well — under-report these issues. Various issues come into play, including stigma, a sense that little may be done, that there might be repercussions, or that it’s better to just forget about the incident and “drive on” (in military parlance).
In recent research it’s also clear that women veterans in particular are much less likely (by a factor of 4) to report if the perpetrator is in their same military unit.
Another item that needs to be clarified is that both men and women service members, and the transgendered, are susceptible to MST. Some clarification is in order:
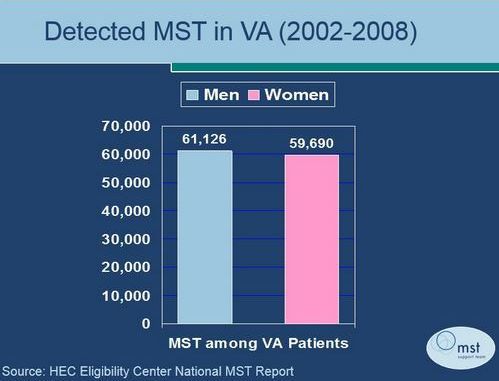
The raw numbers of male and female veterans reporting Military Sexual Trauma (MST) are approximately equal.
- It happens to both male and female service members (see graphic above).
- Because fewer women serve in the military, the prevalence of these incidents happens much more to female service members. Current figures provided on VA’s website are that 25 percent of women and one percent of men seen by VA healthcare report an MST history upon screening by a provider (U.S. Department of Veterans Affairs, 2015).
- (Transgender troops also experience these incidents, but very little research has addressed this small population to date.)
So, the takeaway is:
- Raw numbers of assaults for men and women service members = more or less the same. Percentage of incidents for men and women = vastly different. Women absorb most of those, males fewer. That also means, chances of experiencing them is much greater for women than for men.
- This also means that reporters, advocates and the general public should ask Pentagon to release their sexual assault reports by base by gender, so that we can have a better understanding again of the differences from base to base and uncover some true problem areas.
Getting treatment
Regarding treatment, VA is tasked with providing screening re: MST and also treatment, free of charge, to all veterans who self-disclose that they have suffered MST during their service, without needing to provide documentation about the injury(ies). For historians, this is a somewhat new development, occurring a few years ago — of great potential benefit to veterans.
Some questions to absorb:
- Do MST survivors frequently under-report, perhaps by quite a bit? Yes. Extremely recent research by Blais et al. addresses that. Compared to official figures (27 percent of female veterans), quite a few more women veterans (81 percent) asserted their exposure informally.
- Are male survivors sometimes (although rarely) victims of female perpetrators? Yes, and there’s biology that explains how this happens, though discussing it appears to be taboo. “It’s infuriating that the general public doesn’t understand this issue and doubly disturbing that some advocates add to the stigma and shame by spreading misinformation regarding experiences like mine,” says survivor/advocate James Landrith, who’s devoted thousands of hours trying to make this point clear.
- Do male and female survivors experience the aftermath of the incidents differently? Yes. Anecdotally, male survivors are more likely to question their sexuality and to struggle with suicidal ideation; whereas female survivors are more likely to struggle with depression and social isolation (one reason why in-person support groups are difficult, but not impossible, for female survivors to attend).
- Is there much high-quality material written on this subject? No. Most of the published material to date has been memoirs of survivors, which are very useful for “gaining a picture” of what MST is like to endure, but there are very few sound, well-researched, well-written and comprehensive treatments of the subject from a non-memoir perspective. There are, however, a growing stream of peer-reviewed research articles on the subject which are well worth exploring.
- Does the Pentagon (DoD) release data on the subject by gender? Typically not. Would it be useful if they did? Absolutely. Recently I created a series of data visualizations connected to an article here in Huffington Post, setting out for the first time rates of sexual assault reports by base, based on recent Pentagon numbers. (The reports are a combination of restricted and unrestricted, which is a subject for another time or another expert.) They were not, however, reflective of gender — which is a need for future reporting. (An article linking to all the data visualizations is here.)
- Are MST survivors sometimes also victims of pre-military and even post-military sexual harassment, assault and rape? Sadly, yes. Should this result in victim-blaming? No. But it is a valid element for discussion? Yes. Could DoD do a better, or even a much better, job screening out potential sexual predators? The answer appears sadly appears to be yes.
- Does DoD accept candidates into the military who may have been prior sexual predators? Undoubtedly. Research indicates that answer is yes.
- Does MST complicate and unduly affect future life circumstances? Apparently so (not that that’s surprising, really). Looking only at homelessness, recent research published in 2016 in JAMA Psychiatry indicates that for both male and female veterans, experiencing MST is independently associated with homelessness at every interval they studied — from 30 days to five years out. In my own survey of more than 2,500 women veterans from every era, a full 40 percent of respondents — not all of whom had experienced homelessness — had been told by a healthcare provider that they most likely experienced MST in the military. For that group, incidents of homelessness jumped way up when compared to other women veteran respondents.
- Is it possible there’s an important distinction to be made between “sexual opportunists” and “serial predators” in the military, of whom serial predators are the more important to screen out? (I’m making those terms up, so far as I know, but there’s wisdom behind why this could matter — in terms of impact, ability to deter, and potential number of victims.)
- Does unit culture matter? Yup, apparently. From two key subject matter experts, one from the research world, one from the lived reality/military world, YES. Units that tolerate harassment have worse records with assault and worse. In other words, for optimum impact — stop the problem earlier, at its root.
If you want to educate yourself more about the topic, and film is your preference, there are three good documentaries which taken together convey the full picture (Pro tip: Don’t watch them all at once, without a break. Too overwhelming). The films are: “The Invisible War,” “Service: When Women Come Marching Home,” and “Justice Denied.”
NOTE: If you’re in crisis, you can call the Safe Helpline at 1-877-995-5247 to get confidential one-on-one help. Safe Helpline provides 24/7 sexual assault support for the Department of Defense community. You can also contact the MST coordinator at your local VA Healthcare facility, or reach out to a Vet Center near you.
