Six weeks ago, my family went on a much-needed, highly-anticipated vacation from the polar vortex of Boston to the sunny beaches of Florida. Turns out it was six weeks and a lifetime ago. It was the last time my husband and I slept under the same roof as our three kids; the last time, for that matter, my husband and I spent even five minutes in a room by ourselves; and the last time our 9-year-old daughter slept freely, unencumbered by tubes in her nose, IVs in her arms and the lifeline that now attaches her to a ventilator.
What happened should have been a non-event; our daughter caught a cold. But when you have an underlying mitochondrial disease such as our daughter's, there's actually nothing common about a cold. Weak muscles can make coughing nearly impossible, and if you can't cough you can't clear your secretions. With nowhere else to go, all of the goo that healthy people cough and sneeze out of their bodies stays inside and can end up in the lungs. And now your cold is pneumonia and now your airway is blocked and now you are intubated.
Sure, we'd heard our share of horror stories, but nothing even close had ever happened to us. So, when I calmly took my daughter to the emergency room in Florida, having told my husband to save us a good spot by the pool, it never crossed my mind that we'd be immediately transferred and admitted to the intensive care unite at the local children's hospital -- I'd been expecting a prescription for some antibiotics. And even if I'd let my imagination wander, for sure it wouldn't have occurred to me that she'd be intubated the next day and that one week later we'd be flown back to Boston in a tiny medical plane -- where we'd remain in ICU for more than a month.
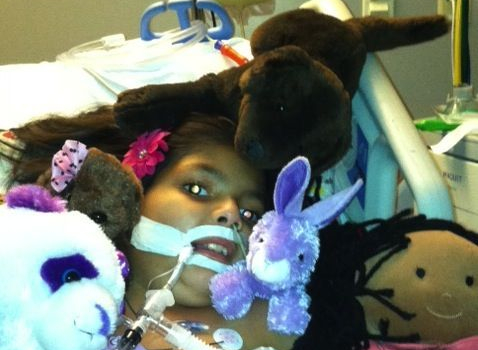
The Pediatric Intensive Care Unit (PICU) is a world unto itself -- separate from the time and space that gives order to our routine lives. It's eerily quiet and deafeningly loud at the same time -- with people talking in hushed voices amidst the cacophony of beeps and alarms that never stop. The rooms are dim throughout the day, but the lights are turned off and on throughout the night as numbers are recorded, medication is administered and vitals are checked. The term "ICU psychosis" is a real one... and I'm beginning to see why.
After six weeks here, I've learned a few things:
1. The doctors may be in charge, but the nurses are running the show.
2. You need to speak up. The respiratory therapists and cardiologists and pulmonologists and neurologists know a lot more about how your daughter's body works than you do, but you know more -- way more -- about your daughter than they ever will.
3. You can learn to speak a new language very quickly when you are motivated. Before long, you will be tossing around terms like "nasal cannula" and "pulmonary toilet" and "gut flora" with the best of them.
4. More patients per nurse is a good thing. If your child has her very own nurse assigned to her, it means your daughter needs her very own nurse.
5. Likewise, don't be worried when the steady stream of doctors coming into your room slows to a trickle... that means things are looking up.
6. People who want to be helpful should just be helpful. Bring a healthy meal to the hospital or some comfort food to the house; take the siblings to a movie; read a book to our daughter so we can leave the room for three minutes. Please don't wait to be asked. We are too tired and too preoccupied to remember to ask.
7. But people who want to be really helpful should do what my friend Ilene did and bring a cozy blanket and new pillow to the hospital. Hospital blankets are the worst.
8. Dark chocolate is also particularly useful.
After all this time, we are beginning to glimpse a light at the end of the tunnel; we're preparing to move to a rehab facility where my daughter can regain her strength and my husband and I can learn to operate some of the equipment that will be coming home with us. But I'm learning -- and this is the hardest of all -- not to get ahead of myself. I've seen one day turn into two and then a week and then six so I try as much as possible to stay in the moment... to celebrate the removal of a tube even if three still remain, to cheer when we get to visit the playroom, even though the IV tower comes with us. And that is a lesson I hope I can hold onto even when we leave the PICU for good.
 Like Us On Facebook |
Like Us On Facebook |
 Follow Us On Twitter |
Follow Us On Twitter |
![]() Contact HuffPost Parents
Contact HuffPost Parents